
Prof Sue Walker AO
MBBS MD FRANZCOG CMFM DDUSue is a maternal fetal medicine specialist and Head of the Department of Perinatal Medicine at the Mercy Hospital for W...
Sleep health is a rapidly evolving field in medicine that recognises that how long we sleep, and how well, are important determinants of health. We are taking these observations from general medicine and asking the question: ‘how they might apply to pregnancy health?’
Sleep-disordered breathing describes all the conditions where the soft tissues at the back of the throat relax during sleep. Snoring is the mildest form of sleep disordered breathing; the most serious is obstructive sleep apnoea. Obstructive sleep apnoea occurs when the upper airway becomes completely blocked during sleep and breathing ceases. The body senses the falling oxygen level and the person is aroused from sleep and re-commences breathing. They then fall back asleep, and the cycle repeats itself. In severe cases, apnoeas (breathing pauses where the oxygen level falls) can occur up to 100 times an hour. In most cases, the person is completely unaware that they stop breathing during their sleep. It is usually when a spouse or family member who draws attention to their snoring that they may think to seek medical advice.
These night-time events have profound impacts on our daytime function and long term health. Chronic sleep deprivation results from being woken from sleep many times per hour overnight. People with severe sleep apnoea have high rates of occupational and traffic accidents as they fall asleep during normal daily activities. These patients also have increased rates of high blood pressure, poor blood vessel health and cardiovascular disease. This is because of the constant damaging effects of low oxygen levels and constant arousal at night on their circulation.
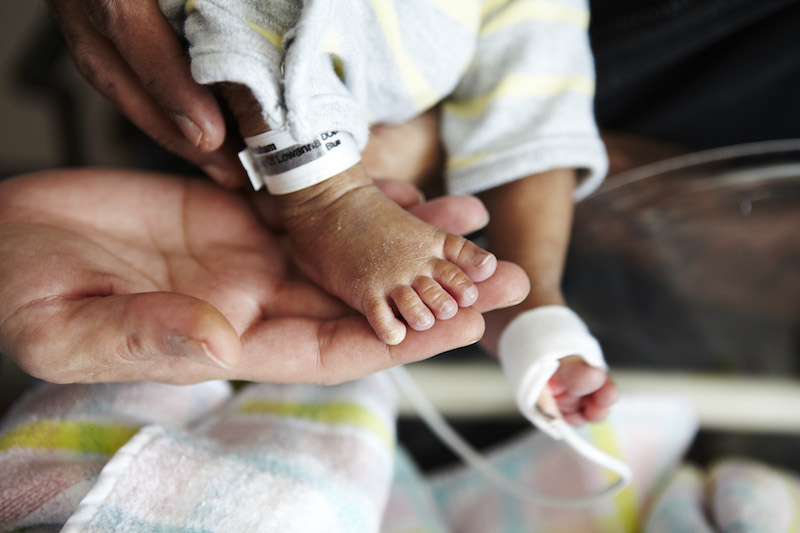
Given the known negative effects of obstructive sleep apnoea in non-pregnant people, we believe that sleep apnoea might play a role in major placental diseases - pre-eclampsia, fetal growth restriction and stillbirth. Uncovering this relationship is now more important than ever, given the current epidemic of obesity. Half of pregnant women attending us for maternity care are now overweight or obese. Obesity is not only a leading risk factor for sleep apnoea, but also for pre-eclampsia, fetal growth restriction and stillbirth. If a link could be found between sleep apnoea and these conditions, it would open exciting avenues for therapy.
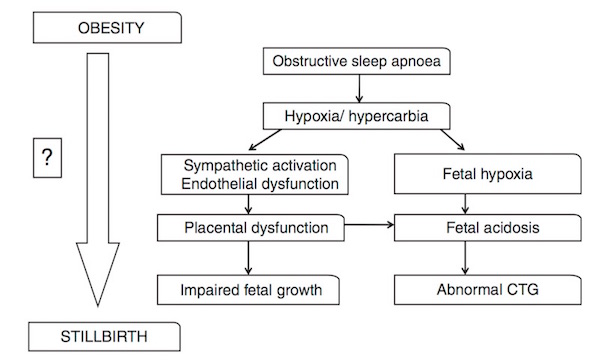
Continuous positive airway pressure (or CPAP) is a safe and effective treatment for sleep apnoea. If there is enough evidence to link sleep apnoea with poor pregnancy outcomes, then CPAP might be a safe and simple means of reducing the maternal and fetal risks faced by obese women during pregnancy.
We are working together with our research partners at the Institute for Breathing and Sleep at Austin Health to study sleep position, blood pressure during sleep, and sleep disordered breathing in pregnancy. We continuously monitor all aspects of the maternal physiology as well as fetal heart rate and movements throughout the night to determine the real-time effect of maternal breathing on the developing baby.
We have received generous financial support from the following funding bodies: